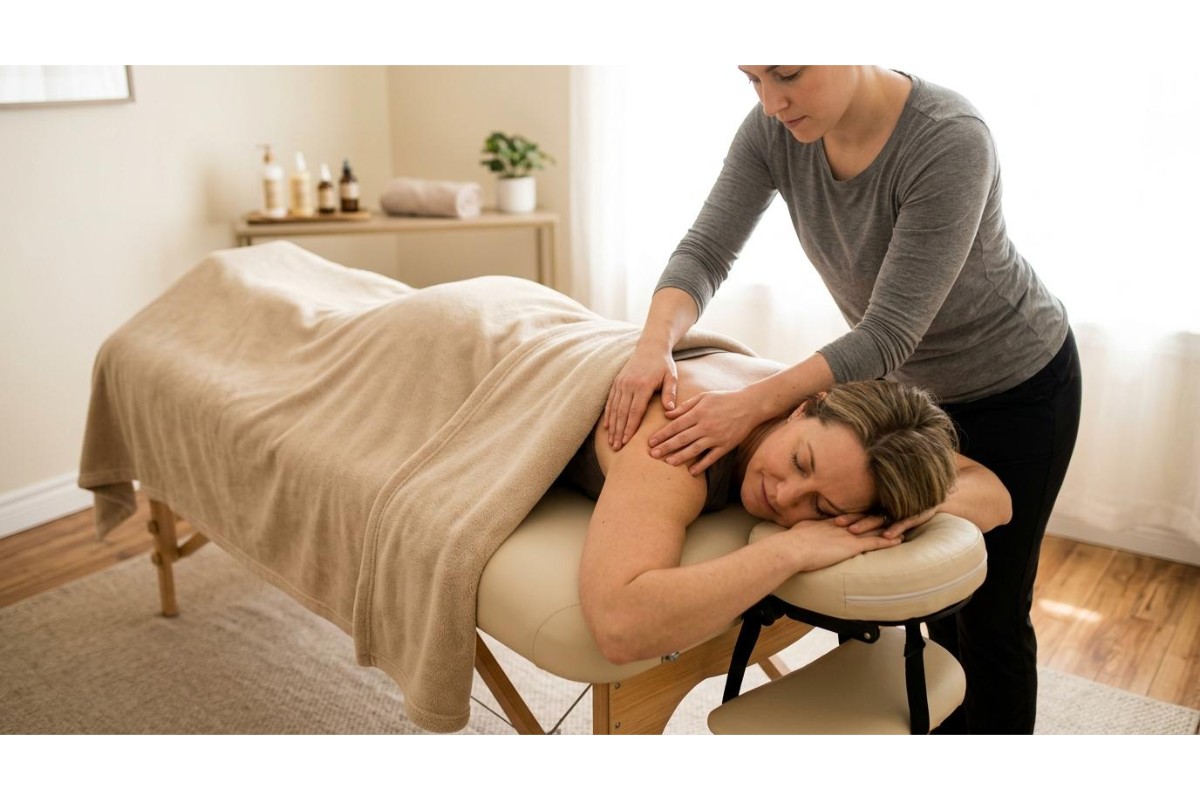
Massage Therapy vs. Physiotherapy: What’s the Difference?
You've been dealing with pain for a while now. Maybe you've tried resting, maybe you've pushed through it, and maybe someone has suggested both massage therapy and physiotherapy, leaving you unsure which one is actually right for you. It's a fair question, and the answer matters when you're trying to get real relief. One to…