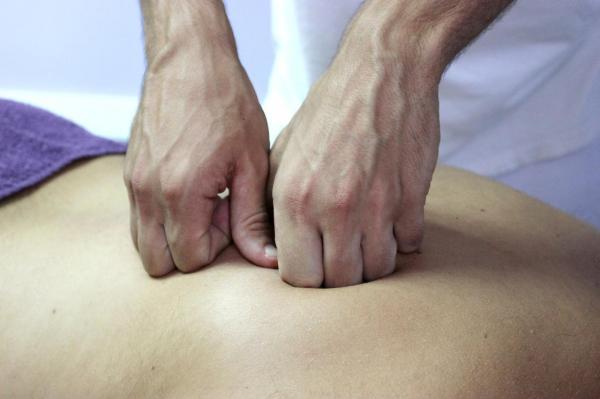
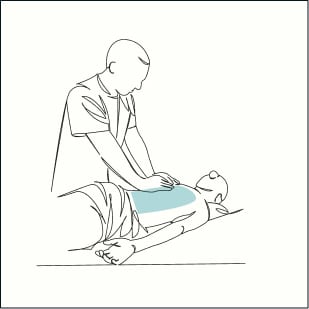
Body Awareness & Your Physical Health
With pain and injuries, we can sometimes dissociate from our bodies. We can get into patterns of ignoring, disliking, getting frustrated with and/or being overprotective and hypervigilant toward our body. There is more and more research showing that practices that promote body awareness are beneficial for overcoming these challenges and improving our health, particularly for…